What Happens When Your Eyes Attack Themselves?
Imagine waking up to find your eyes feel like they've been rubbed with sandpaper, or worse, you can't quite focus them anymore because they're pushing out of their sockets. This isn't just a bad allergy season. It could be Thyroid Eye Disease, which functions as a severe autoimmune reaction where your immune system mistakenly targets the tissue behind your eyes. While many people associate thyroid issues with weight gain or mood swings, the eye complications are often the most frightening part. You might know it as Graves' ophthalmopathy, and while it primarily strikes those with overactive thyroids, it's the swelling and inflammation that cause real damage.
The stakes are high. In moderate-to-severe cases, vision can actually become threatened if the optic nerve gets compressed by swelling muscles. For this reason, understanding the timeline of your symptoms matters immensely. You aren't just dealing with puffy eyes; you are managing a condition that evolves through distinct phases, requiring very different tools depending on whether the fire is still burning or if it's turned into scar tissue.
Spotting the Warning Signs Early
Catching this condition early changes everything. Most patients report a gritty sensation, similar to having dust trapped under your eyelids, reported by nearly 80% of sufferers according to clinical surveys. But that's just the entry-level symptom. If you notice yourself flinching at bright lights or feeling pain when you shift your gaze, these are red flags. About half of all patients experience pain behind the eyes that radiates into the forehead.
Physical changes are equally telling. You might catch your reflection and see your eyes bulging forward, a condition doctors call proptosis. This happens when fat and muscle expand behind the globe of the eye. Another telltale sign is double vision, where looking straight doesn't bring two images together. Interestingly, while many assume this hits one eye first, it usually affects both, though one side can be significantly worse than the other. We categorize these signs using the Clinical Activity Score, a tool that helps experts decide if the disease is "active" and inflamed or "inactive" and fibrotic. If your score is three or higher, that active inflammation requires immediate intervention.
| Symptom Type | Patient Prevalence | Impact Level |
|---|---|---|
| Gritty/Sandy Feeling | 78% | Mild to Moderate |
| Redness & Swelling | 47% | Moderate |
| Double Vision | 28% | High Functional Impact |
| Bulging Eyes (Proptosis) | 31% Severe | Structural Change | r>
Why Does This Happen?
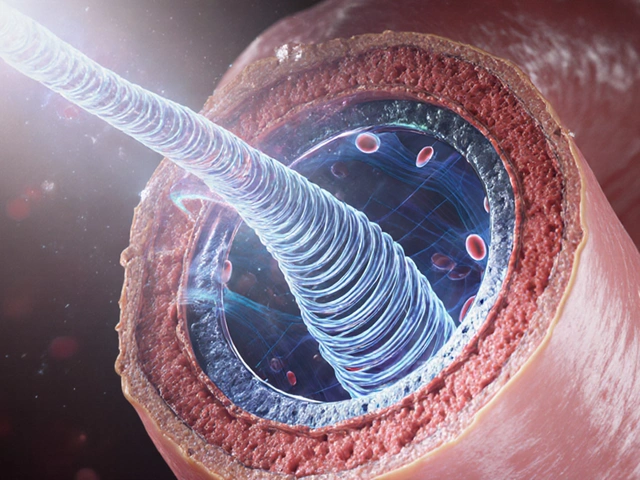
To fix the problem, you have to respect the mechanism. Your body produces antibodies called TSH Receptor Antibodies, which normally regulate thyroid function. In TED, these antibodies travel to your orbit. They bind to cells called fibroblasts located in the retro-orbital tissue-the space behind your eyeball. Once attached, they trigger a chain reaction. This causes normal fat cells to swell and produce more glycosaminoglycans, substances that hold onto water like a sponge. The result? Massive fluid buildup and pressure in a rigid bony box.
This process has two stages. The first is the active inflammatory phase, which typically lasts between 6 to 24 months. During this window, medication works best because you can actually quell the swelling. If you wait too long, the tissue scars down and hardens-this is the inactive or fibrotic phase. Once scarring occurs, drugs won't pull back the retracted tissues; surgery becomes the only option to correct the mechanics. Smoking is a major accelerator here, increasing your risk by nearly eight times. If you smoke, quitting is not just general advice; it's critical survival strategy for preserving your vision.

The Role of Steroids in Active Disease
For decades, corticosteroids have been the heavy artillery used to fight this inflammation. Specifically, intravenous pulse methylprednisolone remains the gold standard for active, moderate-to-severe disease. The protocol is precise: usually 500mg weekly for six weeks, followed by another six weeks at a lower dose. Why IV? Because putting the drug directly into your vein avoids the massive liver metabolism that happens with pills, allowing higher potency to reach the orbital tissue.
This regimen successfully shrinks swollen muscles in about 60-70% of patients. However, it comes with significant baggage. Patients often report rapid weight gain, sometimes upwards of 15 pounds in a few months, along with blood sugar spikes that can push pre-diabetics into full-blown diabetes. There's also the risk of liver toxicity if you exceed cumulative dosage limits (usually capped around 5 grams total). For milder cases, oral prednisone is used, but the relapse rate once you stop taking it is high-around 30%. Because of these side effects, doctors try to reserve steroids for when they are truly necessary to stop sight-threatening pressure.
A New Era: Biologic Treatments
If you've heard nothing else in recent years, hear this: biologic therapies have changed the landscape completely. Until recently, we relied on blunt-force trauma medicine like radiation or steroids. Now, we have targeted weapons. The headline player here is Teprotumumab (brand name Tepezza).
Unlike steroids which dampen the whole immune system, this drug targets a specific receptor: the Insulin-like Growth Factor-1 receptor (IGF-1R). This receptor is overexpressed in the orbital tissue of TED patients. By blocking it, the drug stops the production of the water-retaining sponges mentioned earlier. In the landmark OPTIC clinical trial published in the New England Journal of Medicine, 71% of patients saw their eyes retract by at least 2mm compared to only 20% on placebo. It essentially reverses the bulging.
But there's a trade-off. A full course involves eight infusions over roughly six months and carries a price tag of approximately $360,000 in the United States. Furthermore, side effects are specific. About a quarter of patients report muscle spasms, particularly in the legs, which can be debilitating during exercise. There are also concerns regarding hearing impairment and hyperglycemia. Despite the cost, patient satisfaction rates for biologics sit around 74%, largely because the systemic side effects like moon-face and hair growth associated with steroids are rare.

Treatment Paths and Decision Making
Choosing a path depends entirely on your specific staging. The European Group on Graves' Orbitopathy (EUGOGO) divides the disease into three buckets: mild, moderate-to-severe, and sight-threatening. Mild cases might not need aggressive drugs; artificial tears and selenium supplementation (200mcg daily) can improve quality of life by stopping minor progression. For moderate-to-severe cases, the window of opportunity is the first year of symptoms.
Here is how the logic flows in a specialized center:
- Assessment: Measure proptosis and check for optic neuropathy. Calculate the CAS score.
- Mild Disease: Focus on smoking cessation and local eye care. Add selenium.
- Active Moderate-Severe: Start IV methylprednisolone immediately.
- Steroid Refractory: If steroids fail or side effects are intolerable, switch to Teprotumumab.
- Severe/Sight-Threatening: High-dose IV pulses and potentially urgent orbital decompression surgery to save vision.
One crucial nuance involves radioactive iodine (RAI) treatment for hyperthyroidism. If you need RAI for your thyroid function, doing so can actually trigger or worsen eye disease in 20% of patients. Doctors often prescribe concurrent steroids to shield against this flare-up. Timing your thyroid cure alongside your eye management requires tight coordination between your endocrinologist and your ophthalmologist.
The Human Element of Recovery
Medical data tells one story, but patient experiences tell another. Access to newer biologics remains a massive hurdle. Nearly half of patients report insurance denials before finally getting approval for coverage, creating delays that can be detrimental. One common complaint on patient forums is the financial burden even with insurance, especially given the copays associated with specialty pharmacies.
Emotional health plays a role too. Living with altered facial appearance impacts social interaction and confidence. Some patients describe the bulging as making them feel "alien." Support groups, both online and in-person, provide vital coping mechanisms. Recovery is rarely linear. You might get your protrusion corrected, but then struggle with double vision later as the muscles settle differently. Strabismus surgery to align the eyes often follows medical treatment, scheduled only after the active phase subsides completely.
Where We Are Heading Next
The field is moving fast. Newer agents like satralizumab are showing promise for those who don't respond to teprotumumab, offering subcutaneous injections rather than infusions. Research is currently focused on predictive biomarkers-specifically genetic markers that tell us who is likely to get severe eye disease before symptoms appear. If this succeeds, we could move from reactive treatment to preventative strategies for high-risk individuals. For now, the best defense remains early recognition, smoking cessation, and rapid engagement with a multidisciplinary team that understands both thyroid dynamics and orbital anatomy.
Can Thyroid Eye Disease go away on its own?
Yes, the active inflammation phase eventually settles into an inactive phase, typically within 1 to 3 years. However, while the inflammation stops, permanent structural changes like bulging eyes or scarred muscles often remain without treatment.
Is smoking really that dangerous for TED?
Absolutely. Smoking increases the risk of developing Thyroid Eye Disease by nearly 8 times and makes the condition significantly more severe. It also reduces the effectiveness of treatments like IV steroids.
How much does Tepezza cost without insurance?
A full treatment course involving eight infusions can cost approximately $360,000 in the US without insurance support. Most patients rely on commercial or public insurance plans to cover this expense.
When is surgery needed for eye bulging?
Orbital decompression surgery is typically reserved for the inactive phase of the disease. It is performed to reduce proptosis permanently when medications can no longer shrink the swollen muscles effectively.
Do steroids always work for TED?
No. While effective for many, about 30-40% of patients do not respond adequately to steroids alone, either due to relapse after tapering or inability to tolerate the systemic side effects of the medication.





Philip Wynkoop
really informative stuff regarding the eye inflammation 😅
Debra Brigman
our immune systems are beautiful yet terrifying symphonies of biology when left unchecked. It feels like a visceral betrayal when the body turns its defenses against the very organs that grant sight. We navigate this fragile landscape hoping for equilibrium amidst chaos. There is a poetic tragedy in the swelling tissues behind the globe.
tyler lamarre
Most people here clearly don't understand basic immunology. They read a blog post and think they have cured their disease. Smoking causes damage that steroids simply cannot reverse efficiently. It is amusing to watch these individuals deny personal responsibility. Medical literature clearly states the correlation between nicotine and orbital fibrosis. Yet they prefer to blame the insurance companies instead. One might suggest ignorance is bliss in this particular context. But blindness is not a consequence anyone should take lightly. The drug costs mentioned are astronomical for average earners. The assumption that wealth dictates survival rates seems common. Insurance panels reject claims constantly without valid reasoning. Patients accept the side effects of prednisone without hesitation. Moon faces and hyperglycemia become normal to them overnight. Society pushes expensive biologics while ignoring simple prevention steps. It is frustrating watching the collective denial unfold publicly.
Devon Riley
Hey there friend we need to remember that health journeys vary wildly. People dealing with this condition face real pain daily. Steroids cause difficult changes yes but hope remains strong. Biologics offer new paths forward for many patients. We should focus on empathy instead of judgment. Your support means everything to someone struggling right now. Healing takes time and patience always. 🤗❤️✨
Jordan Marx
From a clinical perspective the EUGOGO classification dictates treatment algorithms. Mild cases warrant selenium supplementation and observation primarily. Moderate severe active phases require IV pulse methylprednisolone protocols immediately. Teprotumumab targets IGF-1R signaling pathways effectively reducing proptosis metrics. Orbital decompression remains the surgical gold standard for fibrotic stages. Coordination between endocrinology and ophthalmology is mandatory. Radioactive iodine therapy demands concurrent steroid coverage to prevent exacerbation. Clinical Activity Score above three signals acute inflammation. Glycosaminoglycan accumulation drives retro-orbital tissue expansion pressure. Multidisciplinary teams manage these complex autoimmune orbitopathy cases best.
kendra 0712
Wow! This section on CAS scores is amazing!!! It explains everything so clearly!! I love how detailed the protocol breakdown is!!! Selenium is such a great tip!! Always consult your doctor first!! Hope everyone finds relief soon!!!
Rohan Kumar
typical big pharma narrative trying to sell $360k treatments 🙄 insurance will deny you regardless. they know the drugs work because the tests are paid for by the same company making the drug 👉 🧠 🚬 💊
Sabrina Herciu
Please understand that insurance denials are common but appeal processes exist. Specialty pharmacy copay assistance programs are available through manufacturers. Coverage varies significantly by region and plan type. Prior authorization is required for most biologic infusions. Patients should document prior failed therapies thoroughly. Appeals can be filed with internal review requests initially. External reviews are possible if internal ones fail. Cost burden analysis is essential before starting therapy.
Monique Louise Hill
You really need to prioritize quitting tobacco products immediately if you have symptoms. Smoking is the biggest preventable cause of severe progression. Ignoring lifestyle factors puts your future vision at unnecessary risk. Health requires discipline and personal accountability. Taking care of yourself matters more than any medication. Please consider your family who depends on your eyesight. 🙅♀️❌👩⚕️
Sarah Klingenberg
That is tough advice but ultimately comes from a place of concern :) Quitting helps recovery immensely though support is key too. Many communities online share resources for cessation safely. Everyone deserves compassion during their healing journey. Let us keep encouraging each other through the hard parts. Smiling helps even on rough days :D